DNA test for genetic predisposition to rheumatoid arthritis
Rheumatoid arthritis is a chronic disease from the group of collagenoses, mainly affecting small joints. The progressive course leads to joint deformation with persistent disability.
by e-mail (anytime):
 EN | USD
EN | USD
by e-mail (anytime):
Rheumatoid arthritis is a chronic disease from the group of collagenoses, mainly affecting small joints. The progressive course leads to joint deformation with persistent disability.
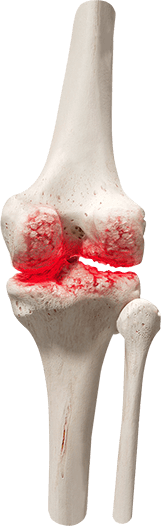

The disease affects around 1% of the whole population of the world, while women ill 4 times more often than men. About 80% of patients suffering from rheumatoid arthritis became ill after 45 years. With each passing year, the risk of developing the disease increases and by the age of 60, it reaches 6% against 0.5-1% for the general population. Juvenile rheumatoid arthritis is diagnosed in children from 2 to 16 years and it's quite rare - no more than 5-7 persons per 10,000 people of the same age.
The mechanism of development of rheumatoid arthritis is based on autoimmune processes associated with a malfunction of immune defense. For a number of reasons, organism start release antibodies (protective cells) begins, which cause a chronic inflammatory process that damages the synovial membrane of joints.
Despite multi-year research, scientists have not been able to identify the exact cause of disease.
Risk factors for rheumatoid arthritis include:
Nowadays, it is recognised that in most cases, rheumatoid arthritis develops against a background of genetic predisposition under the condition of adverse factors.
The value of genetic factor is proved by statistical researches, which show that for patients' close relatives who suffer from rheumatoid arthritis, the risk of disease is 10-12 times higher than the average risk for population in common. For monoval twins the incidence of disease in case of disease of one of them reaches 20%.
There is a whole set of genes coding for a predisposition to the disease, with most of them responsible for the structures of
HLA - a system of histocompatibility, one of the functions of which is recognition and destruction of foreign elements in the body. The most significant is mutation HLA-DR4: it is found in almost 70% of patients with clinically expressed rheumatoid arthritis and only in 25% of healthy people. Other important genes for development of disease are HLA-A10, HLA-DRB1, HLA-Bw6, HLA-B8, HLA-B7, HLA-B27.
Rheumatoid arthritis is a staged disease. The pathological process goes through several stages — prodromal, early, extended and advanced.
In most cases, the first signs of disease develop after previous cold, sinusitis, otitis, or other infectious and inflammatory diseases.
Early symptoms are called prodromal and referred to pre-illness:
feeling of joint stiffness in the morning;
sensitivity to weather changes, which is expressed in pain and aches in joints;
deterioration of well-being;
decreased appetite;
sweating;
slight increase of body temperature.
In a few weeks (sometimes several months), the clinical picture becomes more distinct, while for rheumatoid arthritis the primary lesion of joints of fingers is characteristic, the second in frequency - small joints of feet, and even more rarely- knee, wrist, elbow and ankle joints. In the vast majority of cases, the lesion is of a multiple nature, with a pair of symmetrical joints usually at once involved in the pathological process.
Symptoms of early stage of rheumatoid arthritis:
Edema of the joint.
Redness of the skin above the affected area.
Increased local temperature (joint is hot to the touch).
Pain is almost constant, reinforcing under stress.
At an advanced stage, edema somehow decreases, joints become denser. The articular surfaces are destroyed; the interposition of the phalanges of the fingers is changed. Pain restricts working capacity, prevents sleep, and usually intensifies in the second half of the night and in the morning. The duration of the extended stage is about 1 year.
Pain in the affected joint is reduced, but deformity of joints and severe limitation of their mobility become evident. The characteristic kind of appearance of hands of the patients can be compared with the walrus fins: the fingers in the joints are strongly "turned out". As a result of repeated exacerbations, deformation is aggravated, and the joint becomes completely immobile.
Rheumatoid arthritis refers to systemic diseases: besides joints, skin, muscles and other organs are involved in the pathological process.
Disturbance of skin nourishment:
manifested in dryness, discoloration (pallor, cyanosis), and propensity to trophic ulcers.
Disturbance of nails nourishment:
expressed in brittleness, thinning, deformation of the nail plate.
Rheumatoid nodulus:
appear on the elbows of every fourth patient. These are small painless seals located under the skin, which can increase and adhere to surrounding soft tissues.
Muscular manifestations:
characterized by a decrease in muscle mass in the area of affected joints (amyotrophic syndrome).
Lymph node enlargement:
a response to systemic autoimmune inflammation. Lymph nodes of the neck, submandibular, axillary and inguinal areas can swell, while the general condition worsens, the temperature rises, and body weight decreases.
Cardiovascular disorders:
pain in the heart, signs of arrhythmia may indicate rheumatoid pericarditis. Forming of valvular heart disease is not impossible.
Pulmonary involvement:
most often manifested by pleurisy caused by the formation on the pleura of elements similar to rheumatoid nodules. The patient is disturbed by pain during breathing, fever, severe weakness, shortness of breath.
Kidney symptoms
— pain in the lumbar region, generalized edema and other signs of impaired kidney functions.
Splenomegaly:
a sign of vasculitis - an autoimmune inflammation of small vessels.
Neurological disorders:
neuritis and myelitis, characterized by pain, impaired sensitivity and motor function.
Anemia:
manifests itself in the pallor of the skin, weakness, dizziness, decreased efficiency, etc.
The unfavorable course of the disease is typical for women with a classical onset of the disease after 35 years. Not rare rheumatoid arthritis can progress almost continuously, capturing consistently all small, and then large joints.
Thousands of people all over the world are losing their ability to work in consequence of aggressive course of rheumatoid arthritis. Millions of dollars are spent on treatment and rehabilitation of patients.
Do not wait for the disease, which binds the joints and limits the active life! Take DNA test for a genetic predisposition to rheumatoid arthritis.

To confirm the diagnosis, the following research studies are prescribed:
Radiographic examination of joints:
allows to detect characteristic signs of focal osteoporosis, damage of cartilage and bone tissue, narrowing of joint gap.
Complete blood cell count:
is conducted to identify inflammation markers and determine hemoglobin levels.
Analysis of rheumatoid factor (RF):
characterizes the stage and severity of the process, but it is not strictly specific diagnostic method, as the increase in the index often accompanies other joint diseases. If RFis positive, it is made a diagnosis of seropositive rheumatoid arthritis is, if negative - seronegative rheumatoid arthritis.
Anti-CCP (ACCP)
— a modern immunological method with a high reliability of diagnostics (accuracy up to 90%).
For the diagnosis of vasculitis and other complications, ultrasound, computer tomography, MRI, ECG, articular fluid analysis, arthroscopy and other methods of examination are used.
Timely started treatment is a pledge to prevent severe joint deformities and the development of complications. According to nowadays recommendations, treatment should be prescribed not later than 3 months after the onset of the first symptoms. However, quite often patients are engaged in self-treatment for a long time and thereby worsen the prognosis and their future state.
It should be remembered that the treatment of rheumatoid arthritis with folk medicines, even if reduces the severity of pain syndrome, can not prevent the progression of the inflammation, and hence the increase in deformation and the development of complications are almost inevitable.
For treatment of rheumatoid arthritis, the following drugs are used:
— methotrexate, cyclosporine, sulfasalazine, leflunomide: are the basis of therapy for rheumatoid arthritis. Treatment is prescribed for a long time under the supervision of a specialist. BAID reduces the intensity of autoimmune processes, decreases edema and destruction of articular surfaces.
prescribed for relief of pain and swelling. Drugs do not affect progression of the disease and joint deformity.
are hormonal agents that are used in the severe course of rheumatoid arthritis and low efficacy of BAID. In some cases, intra-articular glucocorticoids are used.
(immunotherapy with infliximab, golimumab, etanercept) is a modern approach in the treatment of rheumatoid arthritis. Drugs of this group aim to block pathological proteins that cause an autoimmune process. If effectiveness is good, immunotherapy usually has fewer and less intensive side effects.
Non-pharmacological methods of treatment that are used are physiotherapy (phonophoresis, electrophoresis, UHF, balneotherapy, etc.), exercise therapy, orthopedic devices. Patients are recommended to eliminate alcohol, avoid infections and stress, and eat well, including in their diet an increased amount of fruits, vegetables, fish. In rare cases, surgical treatment aimed at correcting motor disorders and improving the quality of life is indicated.
Adequate treatment allows reducing the severity of deformity, reducing the frequency and severity of damage to internal organs and significantly improving the patient's well-being.
There is no preventive treatment, all recommendations are as follows:
Prevention of a complicated course of rheumatoid arthritis lies in timely diagnosis and the earliest possible start of adequate treatment. Unfortunately, the clinical picture does not always follow the classical scenario and makes it difficult to make the right diagnosis, in addition, low awareness of the population leads to late seeking medical help.
Take care of yourself and your family! Take the DNA test for a genetic predisposition to rheumatoid arthritis: make prevention the most effective.
